|
Lumbar puncture was performed with a 22-ga needle with the patient in a lateral decubitus position, and a mixture of 0.5 mL of Gadovist (gadobutrol, 1.0 mmol/mL, a nonionic macrocyclic agent Bayer Shering Pharma) or 0.5 mL of Magnograf (gadopentetate dimeglumine, 0.5 mmol/mL Berlis) with 9.5 mL of CSF was administered intrathecally. The unenhanced spine MR imaging protocol included 3 sagittal T2-weighted spin-echo blocks (TR/TE = 4370/93 ms, number of averages = 3, section thickness = 3 mm, FOV = 150 × 300 mm, FOV phase = 50%, flip angle = 150°, acquisition time = 2 minutes and 20 seconds, matrix size = 192 × 512) and 4 sagittal, isotropic 3D heavily T2-weighted turbo spin-echo sequences with fat saturation (FS) (3D T2WI FS) (TR/TE = 1400/180 ms, number of averages = 2, section thickness = 1 mm, FOV = 300 × 300 mm, FOV phase = 100%, flip angle 150°, acquisition time = 4 minutes and 33 seconds, matrix size = 640 × 640) including the entire neurocranium.īefore GdM, written consent for the intrathecal off-label use of a Gd-based contrast agent was obtained from patients. Imaging was performed on a 1.5T scanner (Aera Siemens) using a 20-element head/neck coil and a 32-element table spine coil. Unenhanced spine MR imaging was routinely performed in the morning, and GdM, in the afternoon of the same day. Many patients had been included in previously published studies (study population overlap) investigating different outcome measures, including optic nerve sheath sonography, surgical dural closure, CSF dynamics, DCTM, and brain MR imaging, but none of these studies reported spine MR imaging findings. In the patients participating in a follow-up study (eg, after microsurgical closure or blood patch), only the preoperative examination was evaluated in our study. Patients with a missing spine MR imaging sequence were eligible. The final study population consisted of 103 patients. 
Eighteen patients were excluded because of poor-quality MR imaging or absence of MR imaging. Patients with postdural puncture headache were not included. In total, 121 patients with orthostatic headache and clinical suspicion for SIH were investigated according to our routine diagnostic protocol. Records of all consecutive patients with orthostatic headache and clinical suspicion of SIH evaluated at the University hospital of Bern, Switzerland between February 2013 and October 2017 were retrospectively reviewed. The registry was approved by the local ethics committee (Kantonale Ethikkommission Bern, Switzerland, number: 2017-00861). 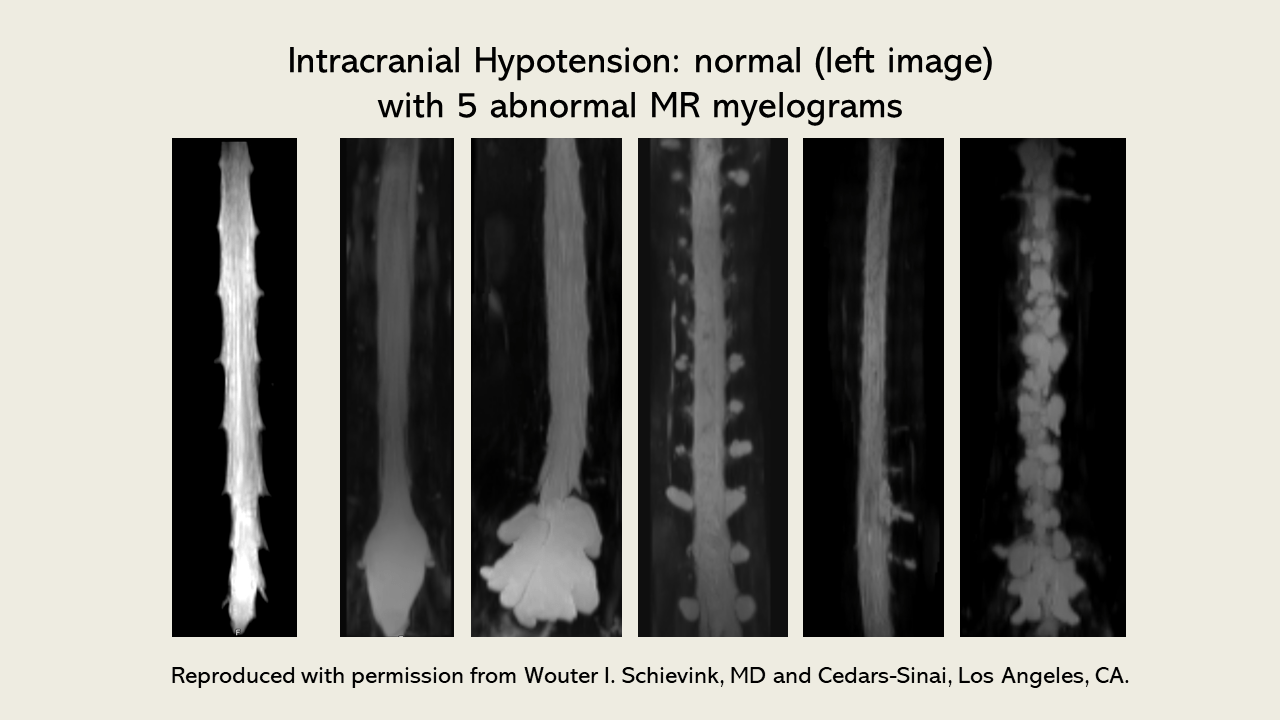
This study was granted institutional review board approval, and the need for informed consent was waived due to its retrospective nature. The goal of our study was to compare the imaging accuracy of 2 different unenhanced spine MR imaging sequences and GdM for visualization of an epidural CSF collection and the accuracy for localizing the precise level of dural dehiscence in the first-line work-up of patients with SIH. Nonetheless, the intrathecal application of Gd has not, so far, been approved by the US Food and Drug Administration and continues to be used off-label. 10 Since then, several studies have reported its utility in the diagnostic work-up of patients with SIH. 8, 9 Adjunctive GdM was first described in 1999 by Zeng et al. Previous reports have indicated the diagnostic value of spine MR imaging. 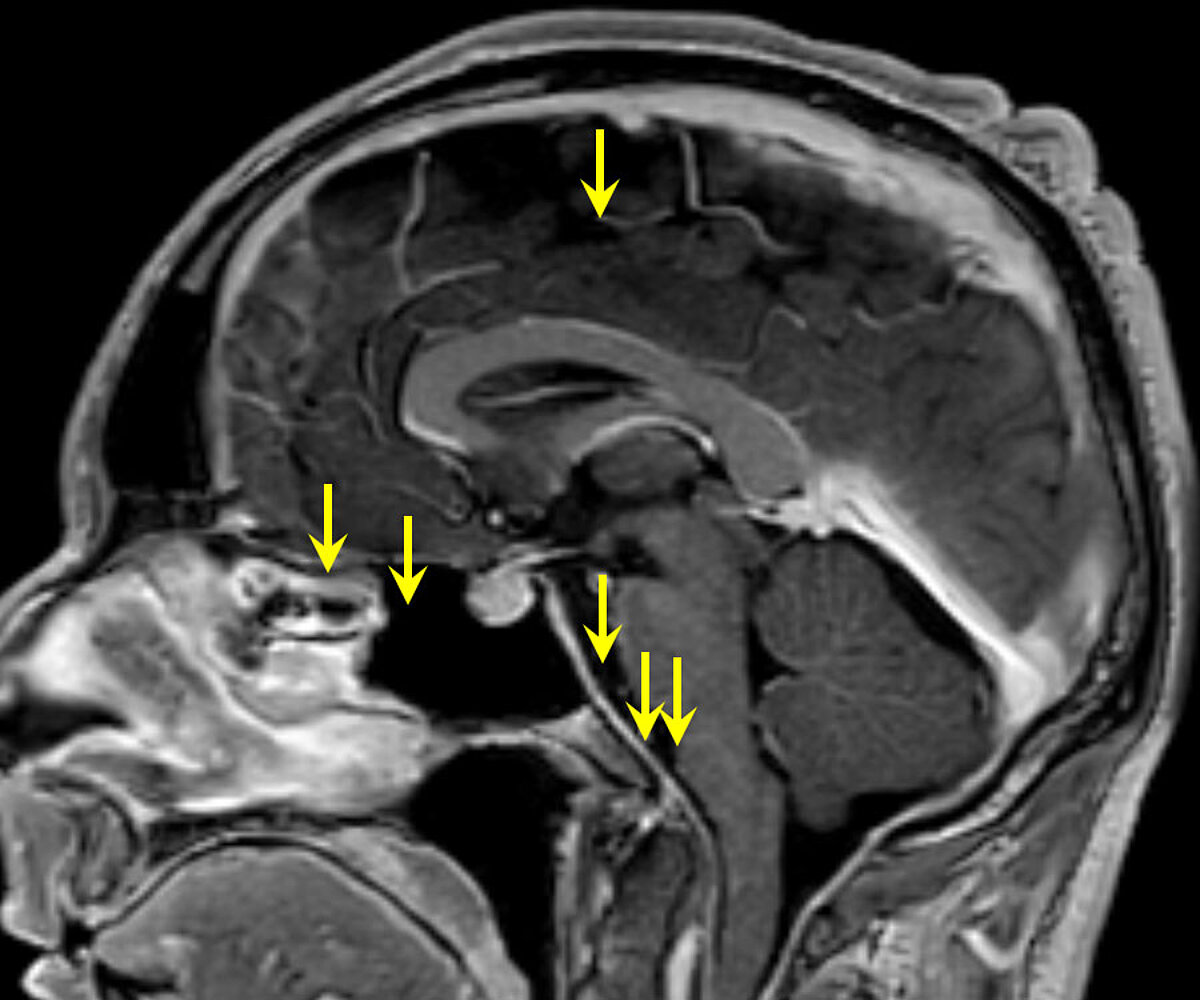
Spine MR imaging plays a key role as the first-line diagnostic examination because it offers excellent spatial resolution without associated radiation exposure however, it lacks any temporal resolution. Each examination has its strengths and shortcomings, and different methods come into play at different stages of the diagnostic process. 4 - 7 Some methods are invasive and require intrathecal application of contrast media, and some may be considered complementary. 
Several radiologic examinations may be used in the spinal diagnostic work-up of patients with SIH and include unenhanced MR imaging, intrathecal gadolinium (Gd) enhanced MR imaging (GdM), conventional dynamic myelography (CDM), postmyelography CT (PMCT), dynamic CT myelography (DCTM), digital subtraction myelography, and radionuclide cisternography. Multiplanar reconstruction of 3D T2WI FS sequence showing a large nerve root diverticulum, which demonstrated a leakage on conventional dynamic myelography (not shown).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
